当科の研修医、山本修輔先生がもやもや病の後大脳動脈の狭窄病変においても内頚動脈系の狭窄病変と同様、外径の縮小(arterial shrinkage)が生じていることを初めて見出し、その論文がWorld Neurosurgery誌に掲載されました。もやもや病の診断精度の向上などに有用と考えています。
A Voyage to Depth of Neuroscience Vol. 58
One of our residents, Dr. Shusuke Yamamoto et al. have published their new article on the arterial shrinkage of the posterior cerebral artery in moyamoya disease.
Yamamoto S, Kashiwazaki D, Uchino H, Saito H, Akioka N, Kuwayama N, Noguchi K, Kuroda S.
World Neurosurg. 2019 Mar 4. [Epub ahead of print]
Stenosis Severity-Dependent Shrinkage of Posterior Cerebral Artery in Moyamoya Disease.
https://www.ncbi.nlm.nih.gov/pubmed/30844529
Abstract
OBJECT:
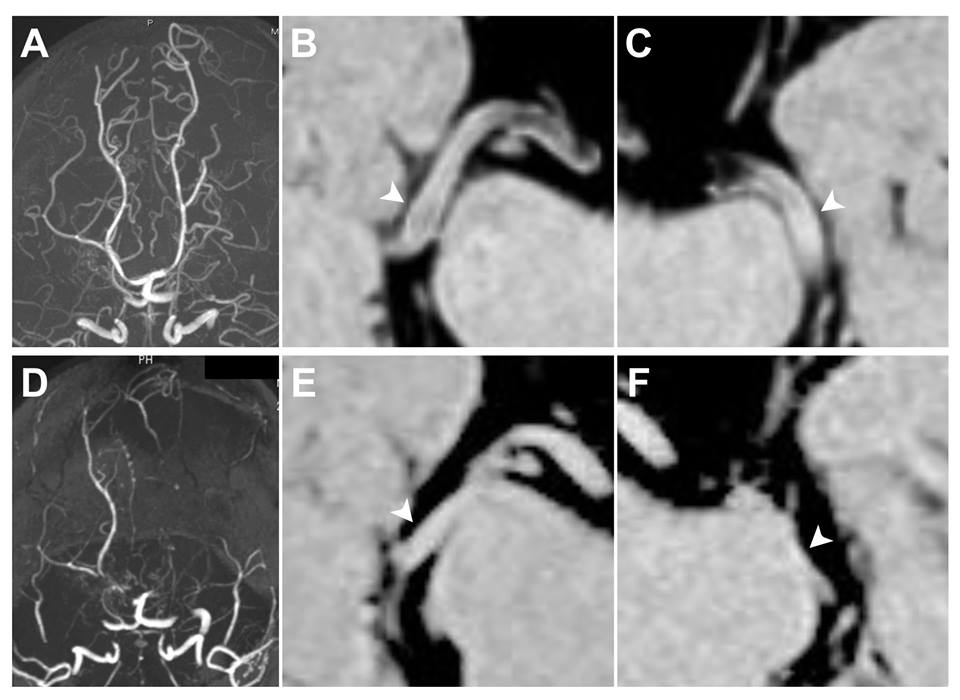
The involved carotid forks in moyamoya disease (MMD) decrease both own luminal calibers and outer diameters. This study was aimed to clarify the changes in outer diameter associated with luminal stenosis/occlusion of posterior cerebral artery (PCA) in MMD.
METHODS:
This study included 24 pediatric and 48 adult patients with MMD and 17 healthy adult controls. Using MR angiography, the degree of PCA involvement was classified into three grades: Grade 0 (normal), Grade 1 (stenotic), and Grade 2 (occluded). Using three-dimensional constructive interference in steady state (3D-CISS), the outer diameters were quantified in the P2 segment. All of them were followed up to identify the disease progression in the PCA.
RESULTS:
The P2 segment significantly decreased the outer diameter with a stepwise fashion in parallel to the severity of luminal stenosis. In pediatric patients, the outer diameters of P2 segments were 2.0±0.26 mm, 1.5±0.42 mm, and 0.87±0.15 mm in Grade 0, 1, 2, respectively (P<0.001). In adult patients, the outer diameters of P2 segments were 2.0±0.34 mm, 1.5±0.34 mm, and 1.1±0.17 mm in Grade 0, 1, 2, respectively (P<0.001). There was no significant difference between Grade-0 PCA of adult patients and healthy controls (P=0.92). Disease progression leaded to further arterial shrinkage of P2 segment (n=4).
CONCLUSION:
The involved PCA demonstrates not only luminal stenosis but also arterial shrinkage in MMD. The finding strongly suggests that the underlying mechanism in the development of MMD is common in both the carotid fork and PCA in MMD.