当科の研修医・山本修輔先生が書いた症例報告がSurgical Neurology International誌に掲載されたのでお知らせします。血行力学的脳虚血をともなう総頚動脈閉塞症に対する脳血行再建術のオプションとして、術前画像の読影がきちんとしていれば、浅側頭動脈−中大脳動脈吻合術(STA-MCA anastomosis)を応用できる症例が存在していることを報告しました。山本修輔先生は卒後3年めですが、これが2本めの英文論文となりました。この調子で診療、研究に邁進してほしいものです。
The Long & Winding Road To Be A Neurosurgeon Vol. 20
Yamamoto S, Kashiwazaki D, Akioka N, Kuwayama N, Kuroda S.
Surg Neurol Int. 2015 Jun 25;6(Suppl 9):S304-8. doi: 10.4103/2152-7806.159377. eCollection 2015.
Superficial temporal artery to middle cerebral artery anastomosis for neovascular glaucoma due to common carotid artery occlusion.
http://www.ncbi.nlm.nih.gov/pubmed/26167375
Dr. S. Yamamoto, a resident at our department, has published his second English-written article in Surgical Neurology International. Following is the abstract:
Background: Common carotid artery (CCA) occlusion sometimes requires surgical revascularization to resolve persistent cerebral/ocular ischemia. High-flow bypass is often indicated in these cases, using the interposed graft such as saphenous vein and radial artery. However, high-flow bypass surgery is invasive and may provide excessive blood flow to ischemic brain. In this report, we present a case that developed neovascular glaucoma due to CCA occlusion and was successfully treated with superficial temporal artery to middle cerebral artery (STA-MCA) anastomosis.
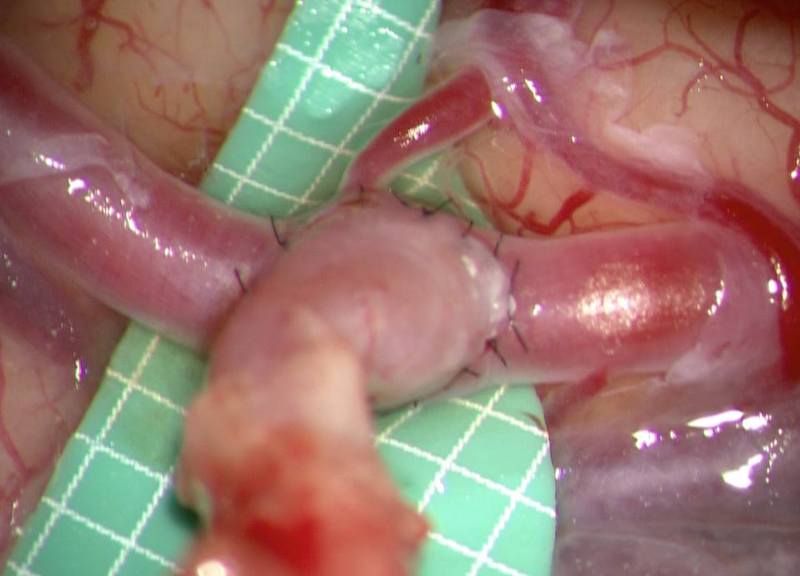
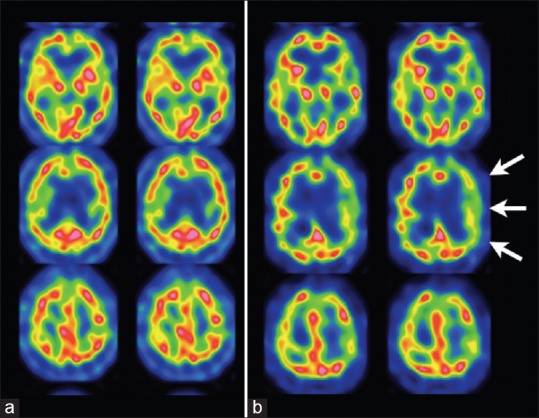
Case Description: A 61-year-old male complained of left visual disturbance and was admitted to our hospital. He underwent carotid endarterectomy for left internal carotid artery stenosis in previous hospital 1-year before, but he experienced left visual disturbance after surgery. Postoperative examinations revealed that the CCA was occluded. His visual disturbance gradually progressed, and he was diagnosed as neovascular glaucoma. None of ophthalmological therapy could improve his symptoms. Blood flow measurement showed an impaired reactivity to acetazolamide in the left cerebral hemisphere. Cerebral angiography demonstrated that the left STA was opacified through the muscular branches from the left deep cervical artery. Therefore, he successfully underwent left STA-MCA double anastomosis. His visual acuity improved and new blood vessels around the iris markedly decreased 3 months after surgery.
Conclusions: Precise radiological examination may enable standard STA-MCA anastomosis even in patients with CCA occlusion.